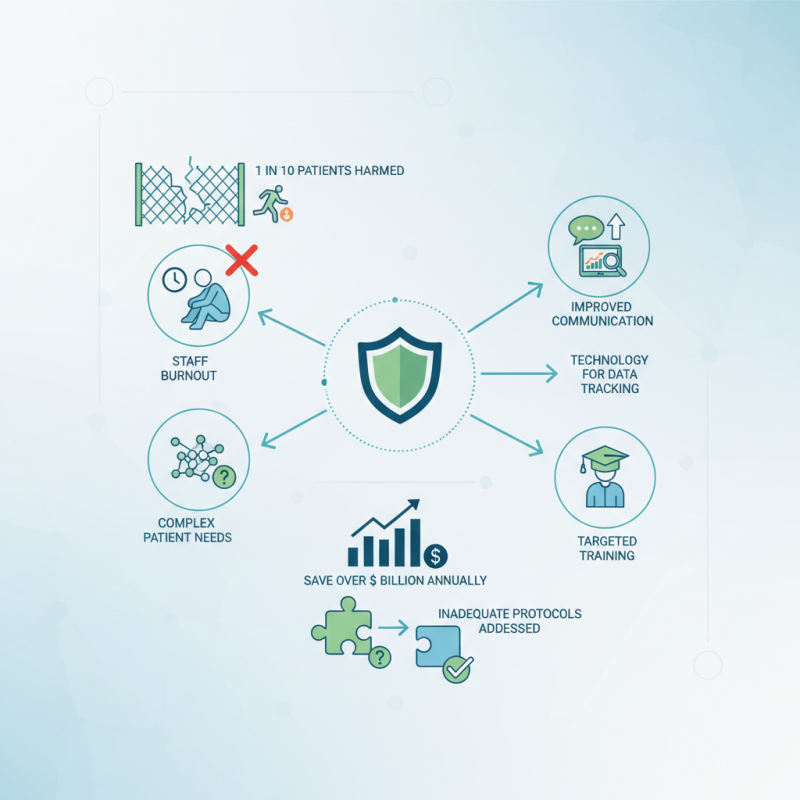
In today's healthcare environment, understanding how to reduce risk in patient care settings is crucial. According to the National Institute of Health, nearly 1 in 10 patients experience harm during their hospital stay. This alarming statistic highlights the need for effective strategies to enhance patient safety.
Health systems must adapt to various challenges, including staff burnout and complex patient needs. A recent report from Healthcare Cost and Utilization Project noted that hospitals could save over $2 billion annually by implementing risk reduction measures. Such measures may include improving communication among staff, utilizing technology to track patient data, and providing targeted training to healthcare workers.
Despite the progress in healthcare, gaps remain in risk management. Notably, studies reveal that a significant number of incidents occur due to inadequate protocols. Addressing these weaknesses is essential. By prioritizing risk awareness and engaging all stakeholders, the healthcare industry can create safer patient care environments.
In patient care settings, risk assessment is crucial for
safety and
quality outcomes.
According to a report from the World Health Organization,
134 million adverse events
occur annually in hospitals across high-income countries. Therefore,
identifying risks early can help mitigate potential harm to patients.
Effective risk assessment begins with comprehensive staff training.
Equip teams with the knowledge to recognize warning signs early.
Regular drills can enhance preparedness for emergencies. Utilizing tools
like Early Warning Scores can aid in identifying deteriorating patients swiftly.
Effective communication among healthcare teams is essential for reducing risks in patient care. According to the Joint Commission, poor communication contributes to over 70% of sentinel events. This statistic underlines the critical need for robust dialogue among healthcare professionals. Clear, direct communication can bridge gaps and enhance patient safety.
Training programs focusing on communication lay the groundwork for effective teamwork. Research shows that teams with structured communication methods experience a 30% increase in patient satisfaction scores. Regular meetings, clear role definitions, and open feedback loops help cultivate a culture of safety.
Healthcare professionals often face challenges in conveying essential information. Misunderstandings can arise, especially in high-pressure situations. Regularly revisiting communication strategies allows teams to identify weaknesses. Reflecting on past interactions can reveal areas for improvement, leading to better patient outcomes. By prioritizing effective communication, healthcare settings can minimize risks and enhance care quality.
In 2026, healthcare relies heavily on technology to enhance patient safety. With advancements in telemedicine and electronic health records (EHR), hospitals can reduce errors. According to a 2023 report by the Institute of Medicine, implementing EHR systems can cut prescription errors by over 40%. This statistic underscores the significance of technology in improving care quality.
Artificial intelligence (AI) is transforming diagnostics. For instance, AI algorithms can analyze imaging data swiftly, reducing human error. A study published in *JAMA* highlighted that AI tools improved diagnostic accuracy by 25%. However, the integration of AI also poses challenges, such as the need for staff training. A flawed implementation can overshadow potential benefits.
Moreover, data security remains a concern. Cybersecurity attacks have increased by 50% in recent years, posing a risk to patient safety. According to the Cybersecurity & Infrastructure Security Agency, healthcare organizations must regularly update their security protocols. Without proper measures, patient data can be compromised. Addressing these concerns is crucial for a safer healthcare environment.
Developing comprehensive training programs for healthcare staff is essential. These programs must focus on risk management and enhance patient safety. Training can help staff identify potential hazards before they escalate. Engaging simulations can provide real-life scenarios for better understanding.
Staff should receive ongoing education, not just initial training. Regular updates on best practices keep the team informed. This approach promotes a culture of safety, urging staff to speak up about concerns. Incorporating feedback from frontline workers is crucial. Their insights reveal gaps in current training methods.
While training is vital, challenges remain. Resources may be limited, affecting program depth. Not all staff respond similarly to training methods. This inconsistency can lead to varying levels of competence. Continuous evaluation of training effectiveness is necessary to ensure improvement. Regular assessments help identify what works and what needs adjustment.
In healthcare, establishing protocols for incident reporting is crucial. These protocols guide staff in identifying and documenting any unusual events. They pave the way for a safer environment for both patients and healthcare providers. However, many facilities struggle with consistent reporting. Barriers often include fear of blame or a lack of understanding of the process.
To improve reporting and response, healthcare teams should prioritize open communication. Encourage discussions during team meetings about recent incidents. This creates a culture of transparency and learning. Consider these tips:
1. Train staff thoroughly on incident reporting protocols. Understanding the process fosters accountability.
2. Create user-friendly reporting tools. Complicated systems discourage staff from reporting incidents.
3. Regularly review and update protocols. Involvement from front-line staff helps ensure these are practical and relevant.
Reflecting on past incidents can lead to valuable insights. Acknowledge that no system is perfect. Mistakes can reveal gaps in protocols. Continuous improvement is essential to enhance patient care and safety.
| Strategy | Description | Impact on Risk Reduction | Implementation Timeline |
|---|---|---|---|
| Standardized Incident Reporting | Implementing a unified system for reporting incidents to improve data collection and analysis. | High - Encourages proactive management of patient safety issues. | 6 months |
| Staff Training and Education | Regular training sessions for staff on incident reporting procedures and patient safety protocols. | Medium - Increases awareness and responsiveness to incidents. | Ongoing |
| Interdisciplinary Team Meetings | Monthly meetings to discuss incidents, share lessons learned, and develop improvement plans. | High - Facilitates collaboration and enhances communication. | 1 month |
| Technology Utilization | Leveraging electronic health records to flag potential safety issues automatically. | High - Reduces human error and improves tracking of patient safety. | 9 months |
| Patient Engagement Initiatives | Encouraging patients to report concerns and participate in their care decisions. | Medium - Empowers patients and increases transparency. | 3 months |
: Risk assessment helps identify potential harm to patients, improving safety and quality outcomes in healthcare.
Comprehensive training equips staff to recognize warning signs early, enhancing emergency preparedness and response.
Implement a feedback system that encourages staff to report near misses, promoting a culture of safety.
Educating patients improves their compliance and satisfaction, reducing the likelihood of adverse events during treatment.
Use simple language and visual aids during education sessions to significantly improve patient comprehension.
Pressure to meet performance metrics can overshadow thorough risk assessments, impacting patient safety.
Technology like EHR reduces prescription errors by facilitating better data management and communication among healthcare providers.
AI tools analyze imaging data quickly, improving diagnostic accuracy but requiring proper staff training to avoid pitfalls.
Data security is crucial, as cybersecurity attacks have surged, highlighting the need for robust security protocols in healthcare settings.
A flawed implementation of technology can overshadow benefits, suggesting the need for careful integration and staff training.
In the quest to understand how to reduce risk in patient care settings, several best practices can be implemented. Firstly, conducting thorough risk assessments is vital to identify potential hazards within the healthcare environment. Effective communication strategies among healthcare teams further enhance patient safety by ensuring all team members are informed and cohesive in their efforts. Utilizing technology, such as electronic health records and decision support systems, reduces the chances of errors and promotes a safer healthcare experience.
Moreover, developing comprehensive training programs for healthcare staff is essential in equipping them with the necessary skills to recognize and respond to risks appropriately. Additionally, establishing clear protocols for incident reporting and response can facilitate swift actions that mitigate the consequences of unforeseen events. By integrating these strategies, healthcare providers can create safer environments for patients and ultimately improve overall care quality.

 Ultrivex Medical
Ultrivex Medical